Diabetes is a chronic condition that affects millions of people worldwide. However, there’s often confusion surrounding the two main types: type 1 and type 2. While both involve blood sugar control issues, the causes, symptoms, and treatments differ significantly.
Understanding the Cause:
- Type 1 Diabetes: This autoimmune disease occurs when the body’s immune system mistakenly attacks the insulin-producing beta cells in the pancreas. This results in little to no insulin production, leaving the body unable to properly regulate blood sugar levels. (Mayo Clinic, Type 1 Diabetes)
- Type 2 Diabetes: This more common form (around 90% of diagnosed cases) develops when the body either becomes resistant to insulin or doesn’t produce enough insulin. (Centers for Disease Control and Prevention, Types of Diabetes)
Identifying the Signs:
Both type 1 and type 2 diabetes can share some symptoms, but the onset and severity can differ:
Type 1 Diabetes: Often develops rapidly in childhood or young adulthood. Symptoms may include:
- Excessive thirst and urination
- Unexplained weight loss
- Extreme hunger
- Fatigue
- Blurred vision
Type 2 Diabetes:
Symptoms may develop gradually and go unnoticed for years. They can include: - Frequent urination
- Increased thirst
- Increased hunger
- Fatigue
- Blurred vision
- Slow-healing wounds
Risk Factors and Early Detection:
While genetics play a role in both types, there are additional risk factors to consider:
Type 1 Diabetes: Family history of type 1 diabetes, certain environmental triggers. There is currently no way to prevent type 1 diabetes.
Type 2 Diabetes: Being overweight or obese, family history of type 2 diabetes, physical inactivity, certain ethnicities, gestational diabetes (diabetes during pregnancy). (American Diabetes Association, Risk Factors for Type 2 Diabetes)
Early detection is crucial for both types of diabetes. Regular checkups and awareness of risk factors can help identify the condition before complications arise.
Treatment Options:
There is no cure for either type of diabetes, but effective treatments can manage blood sugar levels and prevent complications.
Type 1 Diabetes: Requires lifelong insulin therapy delivered through injections, pumps, or continuous glucose monitors (CGM). Maintaining a healthy diet, regular exercise, and blood sugar monitoring are also essential.
Type 2 Diabetes: Treatment varies depending on the severity. It may include lifestyle changes like diet modification and exercise, oral medications, and injectable medications like GLP-1 receptor agonists or SGLT2 inhibitors.
Taking Control of Your Health:
If you experience any diabetes symptoms, consult your doctor for a proper diagnosis. Early detection and proper management can significantly improve your quality of life. Whether you have type 1 or type 2 diabetes, you are not alone. With a dedicated healthcare team, a healthy lifestyle, and access to the latest treatment options, you can effectively manage your diabetes and live a full and healthy life.
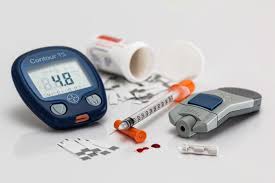
Type 2 Diabetes: Is It Really Reversible?
A recent National Geographic article [link] explores how type 2 diabetes could be reversible with the right approaches. This condition, which affects millions of people worldwide, has long been considered a chronic and progressive disease. However, recent research challenges this perception and suggests that with lifestyle changes and the right approach, remission is possible. The
How Do GLP-1 Drugs Compare? A Breakdown of Ozempic, Mounjaro, and Trulicity
GLP-1 receptor agonists have revolutionized diabetes management, with drugs like Ozempic, Mounjaro, and Trulicity leading the market. But how do these medications compare in terms of effectiveness, side effects, and patient outcomes? Let’s explore their differences and what they mean for diabetes patients. Understanding GLP-1 Medications GLP-1 receptor agonists mimic a natural hormone that helps

Why Has Medicare Spending on Diabetes Medications Skyrocketed in 5 Years?
In the past five years, Medicare spending on diabetes medications has increased nearly fivefold, reaching $35.8 billion in 2023. This surge has been primarily driven by the growing use of GLP-1 drugs such as Ozempic, Mounjaro, and Trulicity. But what is behind this cost escalation, and how does it affect patients and the U.S. healthcare
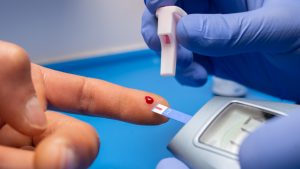
The Gut Microbiota and Blood Sugar Control: A Hidden Connection
The human gut is home to trillions of bacteria that play a crucial role in digestion, immune function, and even metabolism. Recent research has revealed a fascinating link between the gut microbiota and blood sugar regulation, shedding light on how the balance of microbes in our intestines can influence diabetes risk and overall metabolic health.

The Dawn Phenomenon: Why Blood Sugar Rises While You Sleep
For many people with diabetes, waking up with high blood sugar levels can be frustrating—especially if they didn’t eat anything overnight. This early-morning spike in blood glucose is known as the Dawn Phenomenon, and it happens due to natural hormonal changes in the body. But why does it occur, and how can it be managed?

The Influence of Red Light on Blood: Can It Improve Diabetes?
Type 2 diabetes is a metabolic disease characterized by insulin resistance and elevated blood glucose levels. In the search for complementary alternatives to improve glycemic control, red light therapy has gained attention due to its potential to enhance circulation, reduce inflammation, and optimize cellular function. But what does science say about it? ✨ What is

