Diabetes and hypertension are two health conditions that, when present together, can significantly complicate a person’s life. Understanding how to effectively manage both conditions is crucial for maintaining a good quality of life and reducing the risk of serious complications. In this article, we’ll explore the relationship between diabetes and hypertension and offer practical strategies for managing both conditions.
The Relationship Between Diabetes and Hypertension
Diabetes and hypertension are closely linked. People with diabetes have a significantly higher risk of developing hypertension, and vice versa. This relationship is due to several factors:
Insulin Resistance: Insulin resistance, common in type 2 diabetes, can contribute to the development of hypertension. Insulin resistance may lead to increased blood pressure due to changes in blood vessel function.
Inflammation and Oxidative Stress: Both conditions are associated with chronic inflammation and oxidative stress, which can damage blood vessels and contribute to the development of hypertension and cardiovascular issues.
Kidney Complications: Diabetes can cause kidney damage, and damaged kidneys may struggle to regulate blood pressure, exacerbating hypertension.
Strategies for Managing Both Conditions
Managing diabetes and hypertension simultaneously requires a comprehensive approach that addresses both glucose control and blood pressure. Here are some effective strategies for doing so:
1. Regular Monitoring
Glucose Control: Keep track of your blood glucose levels regularly to ensure they are within the range recommended by your healthcare provider. Consistent monitoring can help avoid fluctuations that might affect blood pressure.
Blood Pressure Measurement: Periodically measure your blood pressure to ensure it remains under control. You can use a home blood pressure monitor to keep track between medical visits.
2. Healthy Diet
Low Sodium: Limit sodium intake to help control blood pressure. Opt for fresh, natural foods and avoid processed foods that are often high in salt.
Carbohydrate Control: To manage diabetes, it’s important to control carbohydrate intake. Choose complex carbohydrates and avoid refined sugars that can cause spikes in blood glucose levels.
Potassium-Rich Foods: Foods rich in potassium, such as bananas, spinach, and avocados, can help counteract the effects of sodium on blood pressure.
3. Regular Physical Activity
Aerobic Exercise: Activities like walking, swimming, or cycling can help lower blood pressure and improve glucose control. Aim for at least 150 minutes of moderate exercise per week.
Strength Training: Strength training, such as weight lifting, can also be beneficial for cardiovascular health and blood sugar regulation.
4. Stress Management
Relaxation Techniques: Stress can affect both blood pressure and blood glucose levels. Techniques such as meditation, deep breathing, and yoga can help reduce stress and improve overall well-being.
Counseling and Support: Consider seeking support from a therapist or counselor if stress or anxiety is affecting your health. Emotional management is a key component of managing both conditions.
5. Medications and Treatments
Hypertension Medications: If your doctor prescribes medications for hypertension, be sure to take them as directed. Some hypertension medications may also provide additional benefits for diabetics, such as protecting the kidneys.
Cholesterol Management: Cholesterol-lowering medications may also be necessary if you have diabetes and hypertension, as high cholesterol can increase the risk of heart disease.
Conclusion
Managing diabetes and hypertension simultaneously can be challenging, but with a proactive and coordinated approach, it is possible to keep both conditions under control. The key lies in regular monitoring, a balanced diet, adequate exercise, stress management, and adhering to medical recommendations. Always consult your healthcare team to develop a personalized plan that suits your individual needs.
Remember, taking steps to manage both conditions not only improves your health in the short term but also reduces the risk of long-term complications. Maintain a positive attitude and focus on healthy habits that can help you lead a fulfilling and active life.
E4 Helps you:
At E4, we’re dedicated to revolutionizing how people manage type 2 diabetes through our innovative E4 Alive program. Our team of specialists has joined forces to create a comprehensive solution aimed at empowering individuals to take charge of their health journey. With personalized support and resources tailored to each person’s unique needs, we make managing diabetes simpler and more effective than ever before.
E4 Alive offers a range of tools and resources to help you better understand and control your blood sugar levels. Our program provides personalized guidance to create a healthy eating plan and integrate regular physical activity into your daily routine. Plus, you’ll have access to a supportive community of individuals who understand your challenges and are there to offer encouragement and guidance every step of the way.
By joining E4 Alive, you can effectively manage your blood glucose levels, improve long-term glycemic control, reduce your risk of diabetes-related complications, and enhance your overall quality of life. It’s not just a program; it’s an opportunity to reclaim your health and vitality. Ready to start your journey to better health? Visit THIS PAGE to learn more about E4 Diabetes Solutions and the E4 Alive program.
To learn more about E4 Diabetes Solutions and the E4 Alive program, visit THIS PAGE.
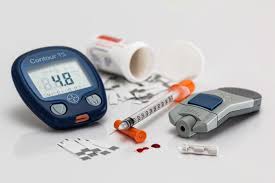
Type 2 Diabetes: Is It Really Reversible?
A recent National Geographic article [link] explores how type 2 diabetes could be reversible with the right approaches. This condition, which affects millions of people worldwide, has long been considered a chronic and progressive disease. However, recent research challenges this perception and suggests that with lifestyle changes and the right approach, remission is possible. The
How Do GLP-1 Drugs Compare? A Breakdown of Ozempic, Mounjaro, and Trulicity
GLP-1 receptor agonists have revolutionized diabetes management, with drugs like Ozempic, Mounjaro, and Trulicity leading the market. But how do these medications compare in terms of effectiveness, side effects, and patient outcomes? Let’s explore their differences and what they mean for diabetes patients. Understanding GLP-1 Medications GLP-1 receptor agonists mimic a natural hormone that helps

Why Has Medicare Spending on Diabetes Medications Skyrocketed in 5 Years?
In the past five years, Medicare spending on diabetes medications has increased nearly fivefold, reaching $35.8 billion in 2023. This surge has been primarily driven by the growing use of GLP-1 drugs such as Ozempic, Mounjaro, and Trulicity. But what is behind this cost escalation, and how does it affect patients and the U.S. healthcare
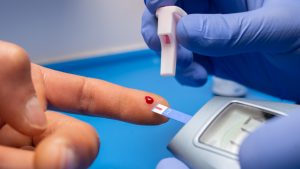
The Gut Microbiota and Blood Sugar Control: A Hidden Connection
The human gut is home to trillions of bacteria that play a crucial role in digestion, immune function, and even metabolism. Recent research has revealed a fascinating link between the gut microbiota and blood sugar regulation, shedding light on how the balance of microbes in our intestines can influence diabetes risk and overall metabolic health.

The Dawn Phenomenon: Why Blood Sugar Rises While You Sleep
For many people with diabetes, waking up with high blood sugar levels can be frustrating—especially if they didn’t eat anything overnight. This early-morning spike in blood glucose is known as the Dawn Phenomenon, and it happens due to natural hormonal changes in the body. But why does it occur, and how can it be managed?

The Influence of Red Light on Blood: Can It Improve Diabetes?
Type 2 diabetes is a metabolic disease characterized by insulin resistance and elevated blood glucose levels. In the search for complementary alternatives to improve glycemic control, red light therapy has gained attention due to its potential to enhance circulation, reduce inflammation, and optimize cellular function. But what does science say about it? ✨ What is

