Pregnancy is a time of remarkable change in a woman’s body, with significant hormonal shifts influencing various aspects of health. One key area affected by these hormonal changes is insulin resistance. Understanding how pregnancy hormones impact insulin resistance is essential for managing your health effectively and ensuring a smooth pregnancy. In this blog, we’ll explore how hormones during pregnancy influence insulin resistance and what you can do to manage these effects.
1. Understanding Insulin Resistance and Hormonal Changes
What is Insulin Resistance?
Insulin resistance occurs when the body’s cells become less responsive to insulin, the hormone responsible for regulating blood glucose levels. This can lead to higher blood sugar levels and, if not managed, may result in conditions such as gestational diabetes.
Hormonal Changes During Pregnancy
Pregnancy involves a surge in several hormones that can affect insulin resistance. These hormonal changes are natural and play crucial roles in supporting fetal development, but they also require careful management to maintain balanced blood sugar levels.
2. Key Hormones and Their Impact on Insulin Resistance
Human Placental Lactogen (HPL)
- Role in Pregnancy: HPL is produced by the placenta and helps ensure the fetus receives adequate glucose by altering the mother’s metabolism.
- Impact on Insulin Sensitivity: Elevated levels of HPL can lead to increased insulin resistance, as the body needs to provide more glucose to the developing baby. This is a natural adaptation to ensure the baby’s growth.
Estrogens and Progesterone
- Role in Pregnancy: These hormones increase significantly during pregnancy. Estrogens support fetal development and maintain pregnancy, while progesterone helps prepare the uterus for the growing baby.
- Impact on Insulin Sensitivity: High levels of estrogens and progesterone can affect how the body responds to insulin. They may lead to a temporary reduction in insulin sensitivity to accommodate the increased energy demands of pregnancy.
Cortisol
- Role in Pregnancy: Cortisol, known as the stress hormone, also rises during pregnancy. It helps regulate metabolism and supports the body’s adaptation to pregnancy.
- Impact on Insulin Sensitivity: Elevated cortisol levels can influence glucose metabolism and insulin resistance. While cortisol is essential for managing stress and energy, its increased levels can contribute to higher blood sugar levels.
3. Managing Insulin Resistance During Pregnancy
Regular Monitoring
- Track Your Blood Glucose: Regular monitoring of blood glucose levels is crucial for keeping insulin resistance in check. This allows for timely adjustments and helps ensure a healthy pregnancy.
- Healthcare Visits: Regular check-ups with your healthcare provider will help you manage insulin resistance effectively and make any necessary adjustments to your care plan.
Healthy Eating Habits
- Choose Low Glycemic Foods: Incorporate foods with a low glycemic index, such as whole grains, vegetables, and lean proteins. These foods help maintain stable blood sugar levels.
- Balanced Meals: Eating smaller, balanced meals throughout the day can help prevent spikes in blood sugar and support overall energy levels.
Exercise and Physical Activity
- Stay Active: Engaging in moderate, safe exercises like walking, swimming, and prenatal yoga can improve insulin sensitivity and overall health.
- Consult Your Doctor: Always talk to your healthcare provider before starting any new exercise regimen to ensure it is safe for you and your baby.
Stress Management
- Practice Relaxation Techniques: Stress can impact insulin sensitivity, so incorporating relaxation techniques like deep breathing, meditation, and gentle stretching can be beneficial.
- Seek Support: Joining support groups or seeking counseling can help manage stress and provide emotional support during pregnancy.
4. Preparing for a Healthy Pregnancy
Preconception Planning
- Health Evaluation: A thorough health check-up before pregnancy helps identify any issues related to insulin resistance and allows for proactive management.
- Lifestyle Adjustments: Adopting a balanced diet and regular exercise routine before conception can support a healthy pregnancy and better manage insulin resistance.
Education and Awareness
- Stay Informed: Learning about how pregnancy hormones affect insulin resistance can help you understand and manage the changes more effectively.
- Join Support Networks: Connecting with others who are managing insulin resistance during pregnancy can provide valuable support and share practical tips.
5. Embracing a Positive Outlook
Celebrate Your Progress
- Acknowledge Your Efforts: Recognize and celebrate the positive steps you’re taking to manage insulin resistance. Each effort contributes to a healthier pregnancy and a positive experience.
Stay Optimistic
- Focus on the Journey: Maintaining a positive outlook and focusing on the supportive resources available can make a significant difference in your pregnancy experience.
6. Conclusion
Understanding how pregnancy hormones affect insulin resistance empowers you to take proactive steps to manage it effectively. By staying informed, adopting healthy habits, and working closely with your healthcare team, you can support a balanced pregnancy and ensure the well-being of both yourself and your baby.
Remember: Always consult with your healthcare provider for personalized advice and support tailored to your needs. With the right approach, you can navigate the changes in insulin resistance during pregnancy with confidence and positivity.
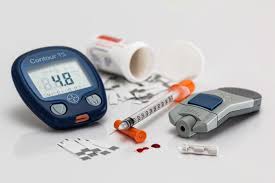
Type 2 Diabetes: Is It Really Reversible?
A recent National Geographic article [link] explores how type 2 diabetes could be reversible with the right approaches. This condition, which affects millions of people worldwide, has long been considered a chronic and progressive disease. However, recent research challenges this perception and suggests that with lifestyle changes and the right approach, remission is possible. The
How Do GLP-1 Drugs Compare? A Breakdown of Ozempic, Mounjaro, and Trulicity
GLP-1 receptor agonists have revolutionized diabetes management, with drugs like Ozempic, Mounjaro, and Trulicity leading the market. But how do these medications compare in terms of effectiveness, side effects, and patient outcomes? Let’s explore their differences and what they mean for diabetes patients. Understanding GLP-1 Medications GLP-1 receptor agonists mimic a natural hormone that helps

Why Has Medicare Spending on Diabetes Medications Skyrocketed in 5 Years?
In the past five years, Medicare spending on diabetes medications has increased nearly fivefold, reaching $35.8 billion in 2023. This surge has been primarily driven by the growing use of GLP-1 drugs such as Ozempic, Mounjaro, and Trulicity. But what is behind this cost escalation, and how does it affect patients and the U.S. healthcare
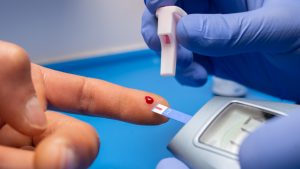
The Gut Microbiota and Blood Sugar Control: A Hidden Connection
The human gut is home to trillions of bacteria that play a crucial role in digestion, immune function, and even metabolism. Recent research has revealed a fascinating link between the gut microbiota and blood sugar regulation, shedding light on how the balance of microbes in our intestines can influence diabetes risk and overall metabolic health.

The Dawn Phenomenon: Why Blood Sugar Rises While You Sleep
For many people with diabetes, waking up with high blood sugar levels can be frustrating—especially if they didn’t eat anything overnight. This early-morning spike in blood glucose is known as the Dawn Phenomenon, and it happens due to natural hormonal changes in the body. But why does it occur, and how can it be managed?

The Influence of Red Light on Blood: Can It Improve Diabetes?
Type 2 diabetes is a metabolic disease characterized by insulin resistance and elevated blood glucose levels. In the search for complementary alternatives to improve glycemic control, red light therapy has gained attention due to its potential to enhance circulation, reduce inflammation, and optimize cellular function. But what does science say about it? ✨ What is

