In recent years, there has been growing recognition of the intricate connection between mental health and physical well-being. One area where this connection is particularly pronounced is in the realm of type 2 diabetes. Research has increasingly shown that neglecting mental health can significantly elevate the risk of developing type 2 diabetes. In this article, we will delve into the various ways in which poor mental health practices can contribute to the onset of type 2 diabetes and explore strategies to mitigate this risk.

Understanding the Connection:
The relationship between mental health and type 2 diabetes is complex and multifaceted. Individuals experiencing chronic stress, anxiety, or depression often resort to unhealthy coping mechanisms such as overeating, sedentary behavior, or substance abuse. These behaviors can lead to weight gain, insulin resistance, and ultimately, the development of type 2 diabetes. Additionally, poor mental health can hinder individuals’ ability to adhere to diabetes management plans, leading to suboptimal glycemic control and increased susceptibility to diabetes-related complications.
The Role of Chronic Stress:
Chronic stress is a significant contributor to the development of type 2 diabetes. When the body is under prolonged stress, it releases hormones such as cortisol and adrenaline, which can raise blood sugar levels. Over time, this can lead to insulin resistance, a key precursor to type 2 diabetes. Moreover, individuals experiencing chronic stress may engage in unhealthy behaviors such as emotional eating or neglecting physical activity, further exacerbating their risk of developing the disease.
Impact of Depression and Anxiety:
Depression and anxiety disorders are also closely linked to type 2 diabetes risk. Studies have shown that individuals with depression are more likely to develop type 2 diabetes compared to those without depression. Similarly, anxiety disorders have been associated with increased insulin resistance and impaired glucose metabolism. The interplay between these mental health conditions and diabetes risk underscores the importance of addressing mental well-being as part of diabetes prevention efforts.
Mitigating the Risk:
To reduce the risk of developing type 2 diabetes associated with neglected mental health, it is essential to prioritize self-care and seek support when needed. This may include:
Stress management techniques: Incorporating stress-reducing activities such as mindfulness meditation, yoga, or deep breathing exercises into daily routines can help mitigate the harmful effects of chronic stress on physical health.
Seeking professional help: Individuals experiencing persistent symptoms of depression or anxiety should seek support from mental health professionals. Therapy, counseling, or medication may be recommended to address underlying mental health issues and reduce diabetes risk.
Healthy lifestyle habits: Adopting a balanced diet, engaging in regular physical activity, and getting an adequate amount of sleep are essential for both mental and physical well-being. These lifestyle changes can help improve mood, reduce stress, and lower the risk of developing type 2 diabetes.
Regular health screenings: Individuals with a family history of type 2 diabetes or those experiencing symptoms of poor mental health should undergo regular health screenings to monitor their blood sugar levels and overall health status. Early detection and intervention can help prevent or delay the onset of type 2 diabetes.
In conclusion, neglecting mental health can significantly increase the risk of developing type 2 diabetes. By prioritizing self-care, seeking support when needed, and adopting healthy lifestyle habits, individuals can mitigate this risk and improve their overall well-being. Taking proactive steps to address mental health is not only crucial for diabetes prevention but also for enhancing quality of life and promoting long-term health and vitality.
Related Studies:
- Association of Depression With Increased Risk of Dementia in Patients With Type 2 Diabetes
- Anxiety and depression in patients with type 2 diabetes mellitus, depending on the method of glycemic control
- Association between depression and development of type 2 diabetes in a large French cohort: the CONSTANCES study
- The impact of depression on the risk of type 2 diabetes: a nationwide population-based cohort study
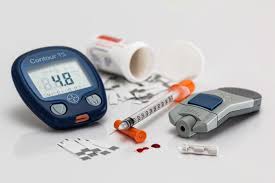
Type 2 Diabetes: Is It Really Reversible?
A recent National Geographic article [link] explores how type 2 diabetes could be reversible with the right approaches. This condition, which affects millions of people worldwide, has long been considered a chronic and progressive disease. However, recent research challenges this perception and suggests that with lifestyle changes and the right approach, remission is possible. The
How Do GLP-1 Drugs Compare? A Breakdown of Ozempic, Mounjaro, and Trulicity
GLP-1 receptor agonists have revolutionized diabetes management, with drugs like Ozempic, Mounjaro, and Trulicity leading the market. But how do these medications compare in terms of effectiveness, side effects, and patient outcomes? Let’s explore their differences and what they mean for diabetes patients. Understanding GLP-1 Medications GLP-1 receptor agonists mimic a natural hormone that helps

Why Has Medicare Spending on Diabetes Medications Skyrocketed in 5 Years?
In the past five years, Medicare spending on diabetes medications has increased nearly fivefold, reaching $35.8 billion in 2023. This surge has been primarily driven by the growing use of GLP-1 drugs such as Ozempic, Mounjaro, and Trulicity. But what is behind this cost escalation, and how does it affect patients and the U.S. healthcare
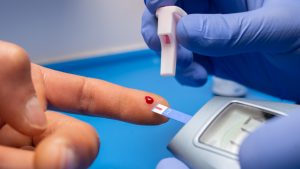
The Gut Microbiota and Blood Sugar Control: A Hidden Connection
The human gut is home to trillions of bacteria that play a crucial role in digestion, immune function, and even metabolism. Recent research has revealed a fascinating link between the gut microbiota and blood sugar regulation, shedding light on how the balance of microbes in our intestines can influence diabetes risk and overall metabolic health.

The Dawn Phenomenon: Why Blood Sugar Rises While You Sleep
For many people with diabetes, waking up with high blood sugar levels can be frustrating—especially if they didn’t eat anything overnight. This early-morning spike in blood glucose is known as the Dawn Phenomenon, and it happens due to natural hormonal changes in the body. But why does it occur, and how can it be managed?

The Influence of Red Light on Blood: Can It Improve Diabetes?
Type 2 diabetes is a metabolic disease characterized by insulin resistance and elevated blood glucose levels. In the search for complementary alternatives to improve glycemic control, red light therapy has gained attention due to its potential to enhance circulation, reduce inflammation, and optimize cellular function. But what does science say about it? ✨ What is

