Type 2 diabetes during pregnancy, also known as gestational diabetes, is a condition that affects a significant number of pregnant women. It is characterized by elevated blood sugar (glucose) levels that are not caused by pre-existing diabetes. While it is usually not permanent, it can lead to complications for both the mother and the baby if not managed properly.

How is type 2 diabetes in pregnancy diagnosed?
In most cases, type 2 diabetes during pregnancy is diagnosed through prenatal screening tests, which are usually performed between 24 and 28 weeks of gestation. These tests may include:
- Oral glucose tolerance test (OGTT): This involves drinking a glucose solution and then measuring blood sugar levels over a two-hour period.
- Random blood sugar test: This measures a blood sugar level at any time of day, regardless of food intake.
What are the symptoms of type 2 diabetes in pregnancy?
While some women with type 2 diabetes during pregnancy experience no symptoms, others may have:
- Frequent urination
- Excessive thirst
- Constant hunger
- Fatigue
- Blurred vision
- Vaginal yeast infections
- Slow wound healing
What are the complications of type 2 diabetes in pregnancy?
If not controlled properly, type 2 diabetes during pregnancy can increase the risk of complications for both the mother and the baby, including:
- Macrosomia: Excessive birth weight of the baby.
- Cesarean delivery: Increased need for a cesarean section.
- Neonatal hypoglycemia: Low blood sugar levels in the baby after birth.
- Preeclampsia: A serious condition characterized by high blood pressure and protein in the urine.
- Type 2 diabetes in the future for the mother: Increased risk of developing type 2 diabetes later in life.
- Childhood obesity: Increased risk of the baby developing obesity and type 2 diabetes in the future.
How is type 2 diabetes in pregnancy treated?
Treatment for type 2 diabetes during pregnancy typically focuses on controlling blood sugar levels through:
- Dietary changes: Adopting a healthy diet rich in fruits, vegetables, whole grains, and lean protein, and limiting processed, sugary, and high-fat foods.
- Regular exercise: Engaging in at least 30 minutes of moderate-intensity physical activity most days of the week.
- Regular blood sugar monitoring: Measuring blood sugar levels regularly, as instructed by your doctor.
- Medication: In some cases, medication may be needed to control blood sugar levels, such as metformin or insulin.
How to prevent type 2 diabetes in pregnancy
While it is not always possible to prevent type 2 diabetes during pregnancy, there are some risk factors you can control, such as:
- Maintaining a healthy weight before and during pregnancy.
- Adopting a healthy diet.
- Engaging in regular physical activity.
- Controlling blood sugar levels if you have a family history of diabetes.
E4: An ally in managing type 2 diabetes in pregnancy
At E4, we have a team of diabetes and pregnancy experts who can provide you with the care and support you need to manage type 2 diabetes during pregnancy. We offer:
- Personalized treatment plans: We develop a treatment plan tailored to your individual needs and those of your baby.
- Education and support: We provide you with information and tools to understand and manage your diabetes.
- Regular monitoring: We closely monitor your blood sugar levels and your baby’s health.
- Comprehensive care: We work together with your obstetrician and other healthcare providers to ensure you receive the best possible care.
Please do not hesitate to contact us if you have any questions or concerns about type 2 diabetes during pregnancy. We are here to help you have a healthy pregnancy and a happy baby.
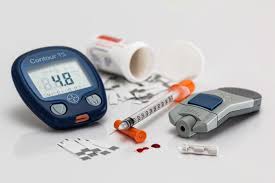
Type 2 Diabetes: Is It Really Reversible?
A recent National Geographic article [link] explores how type 2 diabetes could be reversible with the right approaches. This condition, which affects millions of people worldwide, has long been considered a chronic and progressive disease. However, recent research challenges this perception and suggests that with lifestyle changes and the right approach, remission is possible. The
How Do GLP-1 Drugs Compare? A Breakdown of Ozempic, Mounjaro, and Trulicity
GLP-1 receptor agonists have revolutionized diabetes management, with drugs like Ozempic, Mounjaro, and Trulicity leading the market. But how do these medications compare in terms of effectiveness, side effects, and patient outcomes? Let’s explore their differences and what they mean for diabetes patients. Understanding GLP-1 Medications GLP-1 receptor agonists mimic a natural hormone that helps

Why Has Medicare Spending on Diabetes Medications Skyrocketed in 5 Years?
In the past five years, Medicare spending on diabetes medications has increased nearly fivefold, reaching $35.8 billion in 2023. This surge has been primarily driven by the growing use of GLP-1 drugs such as Ozempic, Mounjaro, and Trulicity. But what is behind this cost escalation, and how does it affect patients and the U.S. healthcare
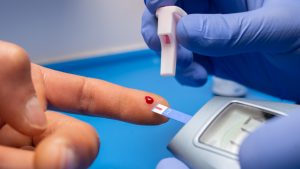
The Gut Microbiota and Blood Sugar Control: A Hidden Connection
The human gut is home to trillions of bacteria that play a crucial role in digestion, immune function, and even metabolism. Recent research has revealed a fascinating link between the gut microbiota and blood sugar regulation, shedding light on how the balance of microbes in our intestines can influence diabetes risk and overall metabolic health.

The Dawn Phenomenon: Why Blood Sugar Rises While You Sleep
For many people with diabetes, waking up with high blood sugar levels can be frustrating—especially if they didn’t eat anything overnight. This early-morning spike in blood glucose is known as the Dawn Phenomenon, and it happens due to natural hormonal changes in the body. But why does it occur, and how can it be managed?

The Influence of Red Light on Blood: Can It Improve Diabetes?
Type 2 diabetes is a metabolic disease characterized by insulin resistance and elevated blood glucose levels. In the search for complementary alternatives to improve glycemic control, red light therapy has gained attention due to its potential to enhance circulation, reduce inflammation, and optimize cellular function. But what does science say about it? ✨ What is

